 Listen to rales here on the Medzcool YouTube channel. Rales are usually broken up into more specific types, based on the way they sound. When these tiny sacs are damaged or weighed down with fluid or mucus, they can make a crackling sound as they attempt to fill with air. These are tiny sacs of air and inflate and deflate with each breath. This usually occurs in the smaller parts of the lungs, like the alveoli. These sounds are formed when air moves into closed spaces. The terms rales or crackles have been used interchangeably and are usually a matter of preference, not a difference in the condition. 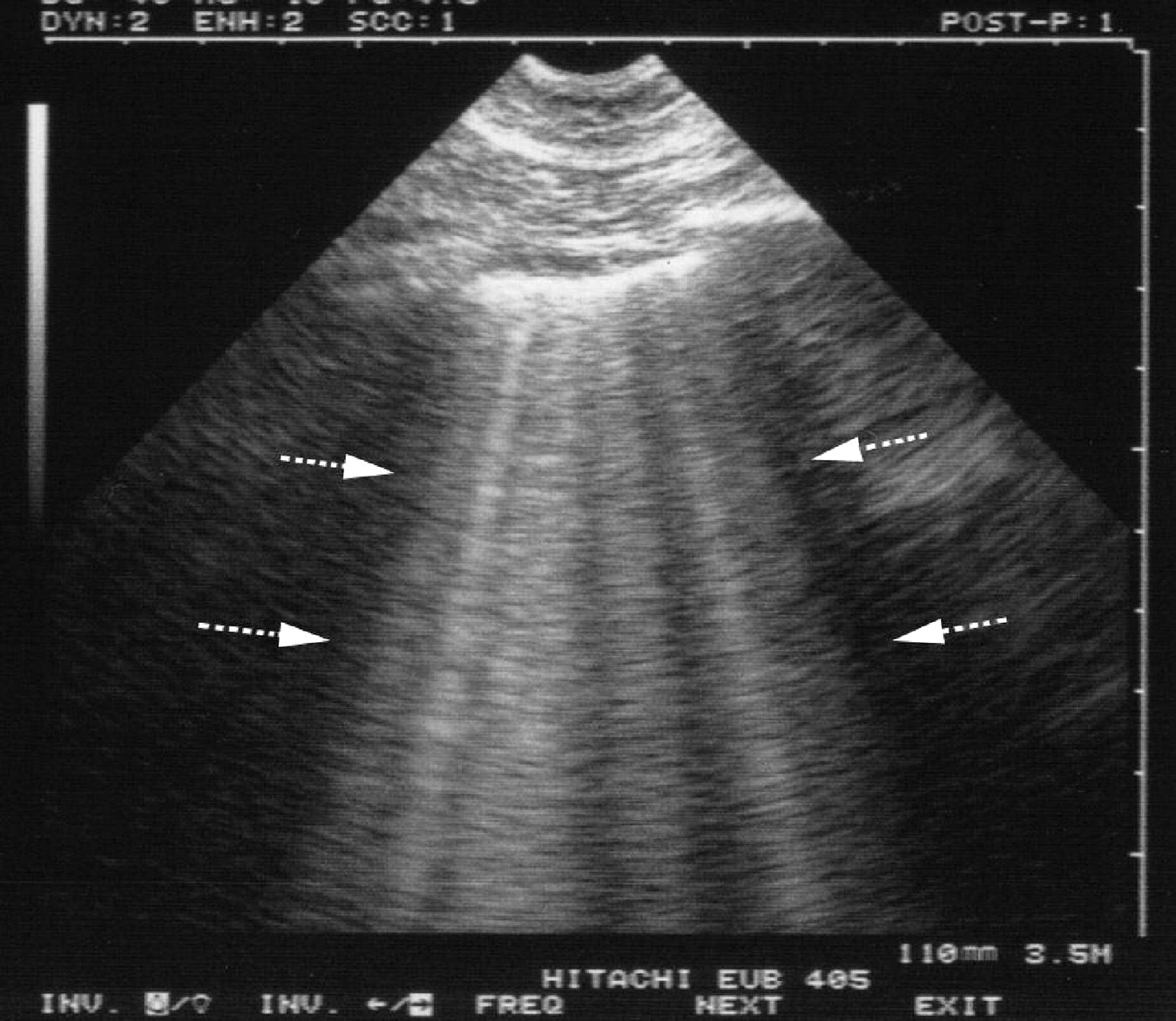
Rales are a higher-pitched sound sometimes called crackles or bibasilar crackles. The chest and the patients breathing pattern are then inspected, followed by. Listen to rhonchi here on the Medzcool YouTube channel. The physical examination of the pulmonary system begins with the patient seated comfortably on the examination table and his/her upper body completely exposed. The sound you hear is the the sound the air makes as it moves around the blockage. These sounds are produced when there is something blocking the airway, like fluid. Rhonchi can either come and go on and inhale or exhale or be heard continuously. It can be heard on an inhale or exhale, and it’s often compared to the sound of snoring. This low-pitched sound that usually starts in the larger airways in the lungs. The difference between the two is in the pitch and the exact cause of the sound. Assess for aortic and mitral valve dysfunction.Rales and rhonchi can both be coarse, even crackling sounds.Assess left ventricular function, ideally systolic and diastolic.Explore the posterior costophrenic angles for fluid.Bilateral small to moderate pleural effusions are common particularly in cariogenic pulmonary oedema.Patients with cardiogenic pulmonary edema may also have obvious cardiac abnormalities on auscultation, such as a murmur or arrhythmia. Interstitial thickening due to fibrosis or lymphangitis can also create the sonographic appearance of diffuse B-lines. Characteristic signs in an animal with pulmonary parenchymal disease often include abnormally loud breathing sounds on thoracic auscultation, such as harsh lung sounds, crackles, and wheezes.Cardiogenic and noncardiogenic oedema may have very similar appearances.These foci may be interstitial or alveolar. They are caused by ultrasound energy reverberating in a fluid filled focus that is surrounded by air.Where there are numerous B-lines in close proximity they become confluent.More than 3 B-lines in any single view is considered pathological.Occasional B-lines are considered normal.Vertical echogenic short path reverberation artefacts originating at the pleural line and extending to the deepest part of the ultrasound image.The ultrasound appearance of pulmonary oedema 
Typical ultrasound features of pulmonary oedema Sometimes the distribution can be useful in differentiating the cause. The clinician must differentiate other causes based on the history and the clinical features of the presentation. Echocardiography can be invaluable in determining the various cardiac causes. Ultrasound can be used to determine the severity and distribution of oedema but not necessarily the aetiology. The ultrasound features of pulmonary oedema are characteristic, but non-specific. Post overdose pulmonary oedema – opiate and salicylate.Post pulmonary embolism pulmonary oedema.19 < 3 B-lines within an intercostal space is considered normal. Re-expansion pulmonary oedema – post large effusion drainage. B-lines Occur due to multiple reflections of sound waves trapped between air and water-rich structures of pulmonary interstitium 1-2 B-lines may be detected in dependent regions of normal aerated lung.Wheezing may be heard, and while many people equate wheezing with. Acute respiratory distress syndrome (ARDS). Listening to the lungs may reveal abnormal lung sounds consistent with fluid accumulation.Noncardiogenic pulmonary oedema occurs most commonly when there is increased permeability of the pulmonary capillaries.Ĭauses of noncardiogenic pulmonary oedema include: 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
